As with other high-incidence cancers, the EOC model of care in the care of the lung cancer patient is the Specialty Oncology Centers (COS), the most modern and effective response to cancer disease.
Lung oncology
Lung cancer is an oncologic disease that is taken care of in the EOC by a dedicated team of specialists at the Swiss Italian Lung Center. Specific organ care, multidisciplinary care, coordination of all phases of the clinical pathway and the advanced technologies available at the center offer the best treatment options today. The Lung Center of Italian Switzerland was awarded the prestigious European Quality Certification in 2023 as a guarantee of its commitment to excellence in the care of oncology patients in Italian Switzerland.
The specialty
The Oncology Center
Centers of expertise structured by organ, EOCs organize and optimize the care of the patient with cancer disease in a multidisciplinary and interprofessional care network. The model involves the cross-disciplinary and coordinated involvement of professionals with complementary specialties, the centralization of highly specialized services, and an accompanying service to treatment and recovery in all EOC hospitals.
Thanks to this model of care, EOC offers all Ticino patients up-to-date treatment protocols on the highest international standards and access to the best diagnostic, therapeutic and care pathway.
What we treat
- Lung cancer: can be broadly classified into two categories, namely small-cell (SCLC) and non-small-cell (NSCLC). The second group can be further divided according to cell differentiation. In addition to morphology, there are other cellular markers that are important in assessing the behavior of the tumor, its biology and, consequently, the most appropriate treatments.
- Other, rarer thoracic tumors:
- Primary malignant tumor of the pleura (mesothelioma).
- Tumors of other organs metastatic to pleura and lung.
- Primary tumors of the thymus (thymomas).
- Other tumors of thoracic organs.
Diagnosis and treatment
Diagnosis
In the case of a suspected pulmonary neoplasm, the patient begins a diagnostic course that defines the characteristics and stage of disease. The different stages include:
- Clinical examination and assessment of any co-morbidities.
- Assessment of pulmonary function and exercise capacity in the case of surgically treatable disease.
- Evaluation of radiological documentation (Rx and chest CT).
- Scheduling and performance ofdiagnostic biopsy examination.
- Staging by PET/TAC and brain MRI.
At the time when the clinician (the attending physician or pulmonologist for example) poses a suspicion of pulmonary neoplasm, based on the patient's symptoms or risk factors, further investigation with a radiological examination is necessary. Radiological diagnostics makes use of the following tools:
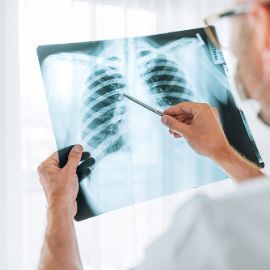
- Chest X-ray: this is generally the first radiological investigation performed in cases of respiratory disorders and allows for the detection of, for example, pneumonia, pleural effusion, or a neoplastic mass. Normal tissue overlap may mask the presence of small nodules. Further investigation with CT examination may be necessary.
- CT scan of the thorax without and/or with contrast medium: this is a second-level examination performed if pulmonary or pleural neoplasia is suspected, to confirm its presence and to check whether the disease is in early or locally advanced stages.
- MRI of the chest with contrast medium: is performed in selected cases if infiltration of structures such as the heart or large vessels is suspected, to decide whether surgery to remove the tumor is possible.
Biopsy sampling is the pivotal moment in the diagnosis of a lung neoplasm. It can be:
- Performed endoscopically: bronchoscopy-EBUS-radial probe.
- Via transthoracic biopsy under CT guidance.
- Via surgical lung biopsy by thoracoscopic route.
- Transbronchial lung biopsy.
- Transbronchial biopsy of mediastinal lymph nodes.
- Surgical lung biopsy.
These examinations allow tissue samples to be taken, larger or smaller depending on the type of sampling, which are analyzed under a microscope for the presence of cancerous cells. Then, at the request of oncologists, molecular analyses are performed to detect any alterations in genes and proteins targeted by specific chemotherapy treatments.
Treatments
The development of warning symptoms of lung cancer is, as a rule, quite late and, therefore, only 30-50% of patients are operable at diagnosis. However, medical advances in recent years have made it possible to offer effective treatments for most patients.
- Surgery is the mainstay of radical treatment and can be offered first or as a complement to other types of therapies. The lung consists of increasingly fine branches of bronchi, arteries and veins, so much so that it can be represented by a tree. Any lung resection must take into account its anatomy.
- Anatomic lung surgery:
- The most frequently proposed surgery is lobectomy, which is the removal of a portion of the lung that represents a morpho-functional unit.
- The extent of resection may be limited to one lobe, two lobes, or the entire lung.
- Recent advances in the technical field, allow us to propose, in certain cases, even more limited operations that are called segmentectomy.
- Non-anatomic lung surgery: we speak in this case of "wedge" or "slice." Wedges are small lung resections that are proposed for diagnosis or treatment of metastases or in cases of limited respiratory function.
- Other surgeries that are reserved for thoracic organ tumors are:
- Thymectomy.
- Pleural biopsies/pleurodesis.
- Lymph node biopsies/aspiration.
- Anatomic lung surgery:
All of these procedures can be performed by open technique or minimally invasive surgery, depending on the issue. Lung oncology in EOC has both thoracoscopic and robotic techniques available. Each surgery is designed according to the characteristics and location of the tumor and according to the peculiarities of each patient.
- Radio-oncology: radiotherapy, possibly combined with chemotherapy, uses high-energy ionizing radiation to "destroy" cancer cells while trying to safeguard surrounding healthy tissues and organs. It is an outpatient treatment and does not involve invasive procedures. It can have several purposes:
- Curative intent: it is performed for the purpose of radically eliminating all cancer cells in the lung and/or loco-regional lymph nodes affected by the disease (can be performed exclusively or in combination with chemotherapy).
- Postoperative Intent (adjuvant): is performed within a few months after lobectomy and lymphadenectomy surgery in order to reduce risks of loco-regional recurrence, if there are risk factors revealed on definitive postoperative histologic examination (positive margins and/or lymph node capsule overgrowth).
- Preoperative (neo-adjuvant) intent: is performed before surgery (often combined with chemotherapy) in order to reduce tumor disease and make a tumor operable.
- Palliative intent: is performed in patients in whom the disease has spread to other organs and aims to improve/resolve a symptom related to the tumor disease.
- Medical oncology: evaluates the indication for therapy with anticancer drugs that are used in different situations and are also used in combination. The choice of therapy depends on the tumor stage, histologic subtype, and molecular profile of the tumor.
- In localized stage: the addition of chemotherapy (and in some cases immunotherapy) to surgery and/or radiation therapy at curative doses is intended to reduce the risk of disease recurrence.
- In metastatic disease: immunotherapy and chemotherapy form the basis of treatment by blocking the progression of cancer cells at metastatic sites.
- Lung cancers that have particular mutations at the level of specific genes (such as EGFR, ALK, ROS1) can be treated with molecular targeted therapies (target therapy).
In case of tumor recurrence or disease progression during cancer treatment: anticancer drugs are intended to keep the disease under control and slow down its progression.
In order to assess the staging and re-staging of lung cancer after therapy, the following nuclear medicine examinations are performed:
- Bone scintigraphy: a diagnostic method to assess the degree of metabolic activity of the skeleton and to recognize any lesion that causes a district alteration of bone metabolic turnover such as metastatic lesions.
- FDG-PET-CT: nuclear medicine method that highlights tumor lesions as cancer cells exhibit increased glucose metabolism and accumulate F18- FDG.
- Lung scintigraphy: a method used to quantify functional lung reserves pre-surgery.
Professionals in Palliative and Supportive Care are an integral part of the team and fit into the surgical, oncology and radiation treatment plan of care in response to emerging needs.
Patient services
Support services
Clinical and diagnostic services
Dedicated services
Insights
Managing the return home
The clinical expert nurse in the field of lung oncology has the skills to provide useful information to the patient and his or her entourage regarding the homebound phase.
Certifications
Certified European Lung Cancer Centre
In February 2023, the Lung Center of the Italian-speaking part of Switzerland was awarded the "Certified European Lung Cancer Centre" certificate by Oncozert of Deutsche Krebsgesellschaft (DKG). The Certificate is awarded based on adherence to requirements set by international guidelines, and confirms that the therapeutic offering corresponds to the quality, practices and methodologies defined by international experts.
Quality and safety of care
Multidisciplinary meetings
Multidisciplinary meetings or multi-disciplinary meetings (MDMs) are a tool developed to further ensure the quality and safety of care provided. In addition to being one of the mandatory requirements for certification, multidisciplinary meetings are intended to ensure that patients have access to the best treatment decisions through the involvement of multiple specialists in the definition and management of pre- and post-operative care.
Cancer League Ticino
In the field of lung oncology, the collaboration with the Cancer League Ticino provides patients with specialized counseling in the social and intensive oncological rehabilitation fields, offering patients and family members advice and support in administrative, financial and other areas.
Through its regional offices (Bellinzona, Locarno, Lugano, Mendrisio), the League is available to all patients and family members for counseling in the social, psychological and rehabilitation fields.
More information is available on the website or by calling 091 820 64 20. Also available is the Cancer Info hotline on 0800 11 88 11 where a nurse with a specialization in the oncology area answers questions from patients and family members in the three national languages.
The League also supports cancer research, offers prevention information campaigns and cooperates with self-help associations.
Doctors
Clinical manager
Doctors on the surgical core team
Contact
Centralized contact management is instrumental in making patient care more efficient, which is still ensured at all EOC sites.
Ambulatorio Oncologia del polmone
Ospedale Regionale di Bellinzona, San Giovanni
-
Orari di risposta al telefono
Monday : 08:00 - 12:00 / 13:30 - 16:00
Tuesday : 08:00 - 12:00 / 13:30 - 16:00
Wednesday : 08:00 - 12:00 / 13:30 - 16:00
Thursday : 08:00 - 12:00 / 13:30 - 16:00
Friday : 08:00 - 12:00 / 13:30 - 16:00
-
Chiusura dell’ambulatorio
Saturday
Sunday
Locations
Lung cancer patients are taken into multidisciplinary care at the Lung Center of Italian Switzerland, which operates at the Regional Hospitals of Bellinzona and Valleys, Lugano, Locarno and Mendrisio.
The English version of this page was created with the aid of automatic translation tools and may contain errors and omissions.
The original version is the page in Italian.