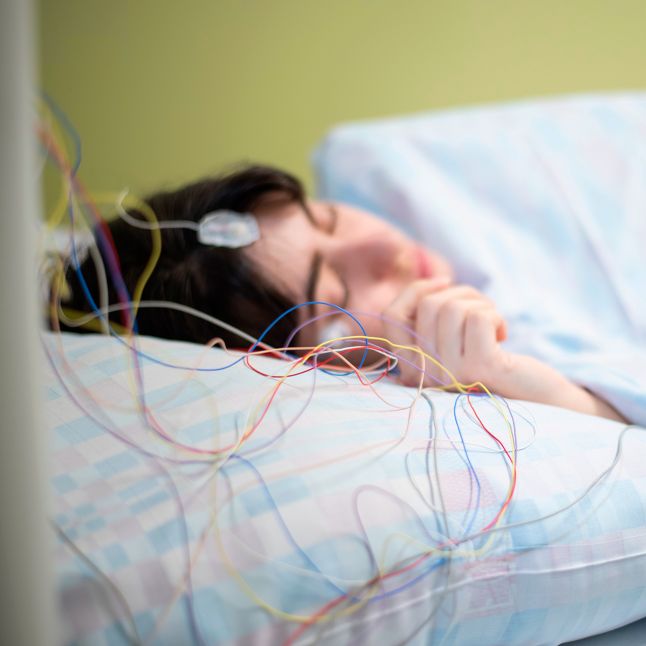
Sleep medicine is a branch of medicine that deals with the diagnosis and treatment in patients of all ages who manifest difficulty initiating or maintaining sleep, excessive daytime sleepiness, respiratory disturbances in sleep, restless leg syndrome, abnormal behavior during sleep, or other sleep-related disorders.
CLINICAL RESEARCH
Clinical Neuroscience and Research
The main research groups in neuroscience are focused on the study of neurodegenerative diseases and neurological disorders.
Go to the dedicated page