clinical research
Oncology and research
The Clinica di Radio-Oncologia is active in the field of clinical research and participates in numerous national and international studies.
Go to the dedicated pageRadiation oncology uses high-energy ionizing radiation to destroy cancer cells and prevent them from multiplying. Used in about one in two cancer patients, radiation therapy is delivered alone or in combination with surgical or chemotherapy treatment, or as palliative treatment.
Patient care is centered on the patient's needs and includes accompaniment through the treatment pathway that precedes and follows radiation therapy. Assisted by physicists, technicians, and nurses, radiation oncology physicians are specialists in the treatment of one or more cancer pathologies and can draw on a broad spectrum of medical and technological expertise to offer personalized, high-precision treatments.
The use of heat for the treatment of cancer has been successfully introduced only in recent decades; in fact, the establishment of the European Society of Oncological Hyperthermia (ESHO), which was deputed to define quality standards and guidelines related to hyperthermic treatments, dates back to 1975. In fact, medical hyperthermia requires advanced technologies that can effectively heat the tumor and closely adjacent tissues in a controlled manner to temperatures between 41°C and 44°C. Hyperthermia works by:
Numerous clinical studies have shown that hyperthermia, when administered with radiotherapy, can increase its efficacy in numerous diseases.
The treatment has rare side effects and does not induce additional toxicities. It generally consists of weekly or biweekly one-hour treatments that are given immediately after radiation therapy treatment. It is performed on an outpatient basis and does not involve invasive procedures other than the placement of temperature sensors in cavitary organs via catheters and/or guides (bladder, rectum, etc.).
Indications:
Each hyperthermia treatment is discussed in an interdisciplinary manner within the Swiss Hyperthermia Network Tumor Board and shared with professionals from other disciplines (medical oncologists, radiologists, nuclear physicians, pathologists, etc.).
The Clinica di Radio-Oncologia EOC has a state-of-the-art technology park capable of ensuring high-precision treatments capable of improving disease control and reducing side effects.
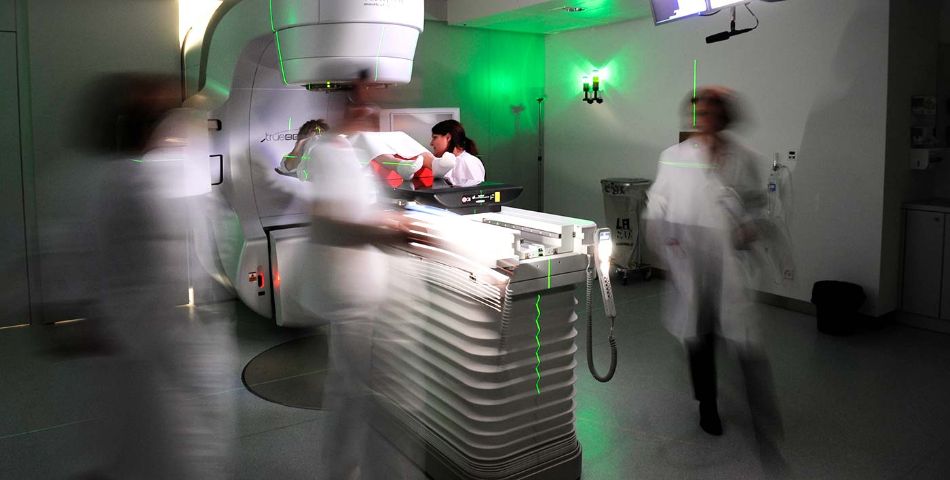
Its technologies feature state-of-the-art machines, including two Varian TrueBeam® linear accelerators for external beam radiotherapy. Equipped with integrated imaging systems(IGRT, Image Guided Radiotherapy), these accelerators are dedicated to the realization of treatments with volumetric technique(VMAT - Volumetric Modulated Arc Therapy), stereotactic (SBRT - Stereotactic Body Radiation Therapy), andradiosurgery(SRS Stereotactic Radiosurgery). These treatments can be carried out in one or more sessions, combining optimal radiotherapy dose distribution with sub-millimeter precision sparing of non-tumor tissues.
These accelerators also integrate the C-RAD® surface imaging system for the realization of treatments synchronized with the respiratory cycle, essential to ensure cardiac and pulmonary protection in breast or lung cancers, and the BrainLab ExacTrac® stereotactic positioning system.
The Clinica di Radio-Oncologia also has an Axxent Xoft® system dedicated to brachytherapy treatments for gynecological tumors, intraoperative treatments(IORT - Intraoperative Radiation Therapy) for breast tumors, and superficial treatments for skin tumors.
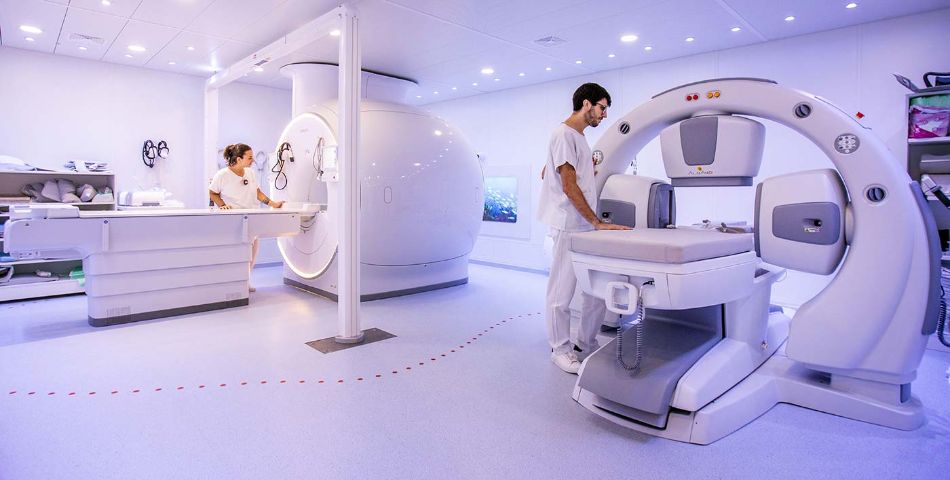
Unique in Ticino and available in only a few national centers of excellence, the Clinica di Radio-Oncologia has been equipped since 2021 with an MRI with a dedicated planning configuration of the latest generation (Philips Ingenia Ambition ®-1.5 Tesla) that allows to improve the accuracy in 'identification of the area to be irradiated avoiding further exposure to ionizing radiation for our patients. Planning MRI is currently used in the planning of specific cancer pathologies (pelvic, urogenital, gynecological, brain, head-neck cancers) as a replacement for conventional CT imaging.
Since 2021, the Clinica di Radio-Oncologia has also been equipped with devices dedicated to the realization ofsuperficial and deep hyperthermia. By emitting radiofrequency electromagnetic waves to deposit energy into tumor tissues causing their temperature to rise, these devices are used in conjunction with standard radiation therapies to improve tumor control.
The two devices used in the Clinica di Radio-Oncologia are:
Clinica di Radio-Oncologia medica since 1992 has been nationally certified by the Swiss Institute for Medical Education (ISFM) and the Federation of Swiss Physicians (FMH) as a Class A training center.
Ospedale Regionale di Lugano, Italiano
Orari di risposta al telefono
Monday :
08:00
- 16:30
Tuesday :
08:00
- 16:30
Wednesday :
08:00
- 16:30
Thursday :
08:00
- 16:30
Friday :
08:00
- 16:30
Chiusura dell’ambulatorio
Saturday
Sunday
Ospedale Regionale di Bellinzona, San Giovanni
Orari di risposta al telefono
Monday :
08:00
- 16:30
Tuesday :
08:00
- 16:30
Wednesday :
08:00
- 16:30
Thursday :
08:00
- 16:30
Friday :
08:00
- 16:30
Chiusura dell’ambulatorio
Saturday
Sunday
Radiation therapy is provided at the Ospedale Regionale di Bellinzona, San Giovanni, and the Ospedale Regionale di Lugano, Italiano.
The English version of this page was created with the aid of automatic translation tools and may contain errors and omissions.
The original version is the page in Italian.
Take just a few moments to share what you think about the new website www.eoc.ch. Your opinions are important to improving everyone's experience.
Fill out the survey now!