Diagnosis
Diagnostics in brain tumors are aimed at multiple purposes:
- To ascertain the oncologic nature of the lesion(s) found in the brain, and at the same time to rule out other causes requiring different treatments.
- To characterize the biological behavior of the tumor, i.e., its degree of aggressiveness, for the selection of the best treatment.
- Determine the precise anatomical location of the lesions, in order to guide surgical and/or radiotherapy treatment to the maximum possible sparing of the areas of the brain responsible for basic functions (movement, speech, vision, etc.).
- Check the effects of different therapies and the identification of any adverse events or complications.
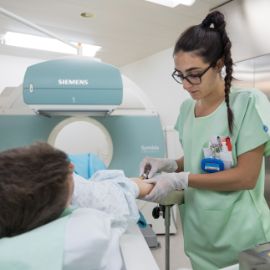
The main examination that is used is multiparametric MRI: using magnetic fields, radiofrequencies, and contrast agent, MRI allows detailed images of the structures of the nervous system to be obtained, which provide many different pieces of information on both the morphology and biological characteristics of brain and spinal tumors. It is used both in the diagnostic phase and in the phase of verifying the effects of treatments, and for these reasons it plays a crucial role throughout the patient care pathway.
The multiple "parameters" correspond to the different types of information, which MRI is able to extract noninvasively through imaging: for example, the density of cells or the amount of blood supplying a tumor may reflect, in certain cases, the degree of aggressiveness of the disease.
Other important tests in diagnosing tumors of the nervous system, provided by the nuclear medicine service, are:
- PET/CT with Fluoroethyltyrosine (FET): useful particularly in gliomas, for metabolic evaluation at diagnosis or for differential diagnosis between disease recurrence and post-treatment changes.
- PET/CT with 68Ga-DOTATATE: particularly useful for evaluation of the extent of complex meningiomas.
In the suspicion of a brain tumor, radiological examinations are essential, but certainty of diagnosis is obtained only by histologic examination, performed in the laboratory by the pathologist, by sampling of tumor cells or tissue by examination of cerebrospinal fluid or biopsy performed by the neurosurgeon.
In order to be evaluated under the microscope, the biopsy is subjected to histochemical staining and immunohistochemical analysis: through analysis of morphology and other features of tumor cells, the type and grade of brain tumor can be classified.
It is also to date necessary to perform an additional level of investigation. Indeed, alterations in the genes and molecules that make up and define the tumor make it possible to identify targets to be hit by radiation and chemotherapy treatments. A recent development in molecular diagnosis concerns the assessment of tumor methylation status (methyloma), which is characteristic for different histotypes. This evaluation allows for confirmation and clarification of the histopathological diagnosis, especially in doubtful cases.